|
9/7/2019 Hemostasis Quizlet
Under normal conditions blood remains fluid and the cellular components of blood, namely erythrocytes, leukocytes and platelets, are not activated or physiologically altered. Similarly the endothelial cells also remain inert.
Only in pathologic conditions is the functional state of these components altered: -Endothelial damage, activation of platelets and release of tissue factor from cells results in thrombogenesis.Once a thrombus is formed it can obstruct blood flow and produce an inflammatory response. 1) Vasoconstriction: a.
Endothlin release b. Reflex vasoconstriction & release of various mediators c. ECM contractile fibers 2) Primary hemostasis: a. Platelets adhere to the damaged vessels (GP Ib binding to vWF).
Platelets undergo shape change, from discoid to non-discoid formation (extending pseudopods). Light granules (alpha) release PF 4, PDGF and other proteins. Dense granules (beta) release ADP, Ca+2, histamine, serotonin and epinephrine.
Describes Briefly What Hemostasis Is. Talks about vasospasm, platelet plug formation and coagulation https://www.facebook.com/ArmandoHasud. Blood: Hemostasis and Blood Coagulation. Click here to study/print these flashcards. Create your own flash cards! Sign up here. Additional Physiology Flashcards. Cards Return to Set Details.
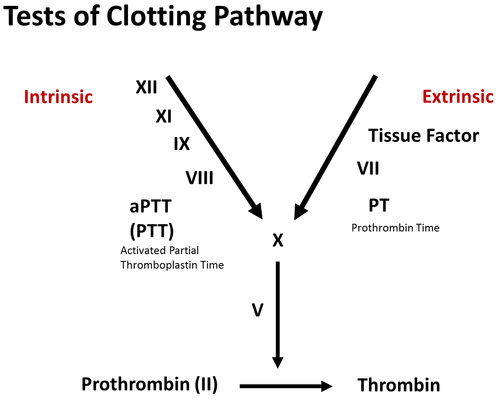
Activated platelets recruit other platelets e. Hemostatic plug formation. Several platelets aggregate and form a plug 3) Secondary hemostasis: a. Tissue factor/Procoagulant released from various cells. Promotes coagulation. Phospholipid complex expression.
Surface phospholipids are expressed. Promote the coagulation process. Thrombin activation. By the activation of coagulation cascade, thrombin is generated.
Fibrin polymerization. The formed fibrin is polymerized by Factor XIIIa. 4) Thrombus and antithrombotic events a) Once the clot is formed, it is subjected to endogenous lysis by fibrinolytic enzymes. Clot size can also be increased due to cellular recruitment. B) The stationary clot (Thrombus) can also break and embolize (Embolus). Platelet adherence and activation: the injury damages endothelial cells and exposes subendothelial collagen - platelets adhere to collagen & become activated - platelets change in shape and release adenosine diphosphate, thromboxane A2 and serotonin - recruit additional platelets to site of injury + promote formation aggregates - hemostatic plug forms Steps: a. Platelets adhere to the damaged vessels (GP Ib binding to vWF).
Platelets undergo shape change, from discoid to non-discoid formation (extending pseudopods). Light granules (alpha) release PF 4, PDGF and other proteins. Dense granules (beta) release ADP, Ca+2, histamine, serotonin and epinephrine. Activated platelets recruit other platelets e. Hemostatic plug formation. Several platelets aggregate and form a plu. Secondary hemostasis: simultaneously, tissue factor is released at the site of injury from the endothelial cells which combine with platelet factors to initiate the plasma coagulation cascade, ultimately forming thrombin.
The coagulation proteins form complexes on the platelet surface utilizing the phospholipids of the platelet membrane. Tissue factor: Procoagulant released from various cells- Promotes coagulation. Phospholipid complex expression. Surface phospholipids are expressed. Promote the coagulation process. Thrombin activation. By the activation of coagulation cascade, thrombin is generated.
Fibrin polymerization. The formed fibrin is polymerized by Factor XIIIa. Formation of platelet-thrombin plug (permanent plug): -Thrombin stimulates recruitment and activation of additional platelets.Thrombin enzymatically converts fibrinogen to fibrin.Fibrin serves to bind (stabilize) and anchor the aggregated platelets. The consolidated platelet-fibrin clot (thrombin) forms a permanent plug which seals the hole in the vessel wall.Erythrocytes and leukocytes become part of the thrombus.Once the clot is formed, it is subjected to endogenous lysis by fibrinolytic enzymes. Clot size can also be increased due to cellular recruitment. The composition of clot depends on the vascular sites and the patients own pathophysiologic state.
Normal endothelial cells inhibit platelet adherence and prevent blood clotting. Injury causes a loss of these anticoagulant mechanisms thereby leading to a pro-thrombotic effect a. Endothelial cells secrete von Willebrand factor (vWF): forms a molecular bridge between platelets and subendothelial collagen - platelet adhesion to endothelial cells occurs. Simultaneously, endothelial cells secrete tissue factor: activates the extrinsic sequence of the coagulation cascade -promotes generation of thrombin and formation of clot, which traps other cells (RBC, leukocytes) -cytokines released by injured endothelial cells can stimulate cells to synthesize more tissue factor. 1) Release of ADP and thromboxane A2 serves to recruit, activate and aggregate greater numbers of platelets into a primary hemostatic plug (temporary plug) 2) Serotonin and thromboxane A2, released by platelet granules, vasoconstrict the vessel, decreasing the size of injury, reducing blood flow and the likelihood of the plug detaching from the vessel wall. 3) Simultaneously, thrombin is formed by the activation of the intrinsic pathway (ADP, calcium, coagulation factors, phospholipid complex). 4) Effects of thrombin: -Thrombin, ADP and thromboxane A2 accelerate platelet aggregation.Thrombin converts fibrinogen to fibrin.Fibrin surrounds and structurally holds platelets in a secondary (irreversible) hemostatic plug.
Comments are closed.
|
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
